Testimonials
REVIEWS OF DR. SCHULER
Advances: in Treatment for Diabetes
Coming Soon!
Coming Soon!
Here are the guidelines for self care that most foot doctor, podiatrist use, and the ones that I have used for about 30 years in my office in Panama City Fl.
People with diabetes can reduce their risk of amputation by following a few qt simple guidelines:
1. Have your doctor check your bare feet at every visit.
2. Cut your toenails straight across when possible. Make sure there are no sharp points left, by using an emery board
3. Wash your feet daily, using warm not hot water.
4. Check them for bumps or sores daily.
5. Use a lotion or moisturizer on your feet to help prevent the skin from cracking or breaking down.
6. Do not wear stockings with seams.
7. Break in new shoes very slowly. Wear them for only one hour a day for the first week, then add an hour to the wearing time every week.
8. Check your shoes every time you put them on, in order to avoid anything that may cause an irritation of the feet to occur.
9. It is not advised to go barefoot due to the nerve loss on the bottom of the feet.
10. When possible cut your toenails straight across, making sure not to leave
an edge that could cut into the other toes.
11. NEVER USE CORN REMOVER, WART REMOVER, OR ANY OTHER CHEMICAL ON YOUR FEET.
12. When bathing check the water temperature with your elbow before
getting in the bath.
13. If your feet stay cold at night wear socks, but do not use hot water bottles, or any other device directly on your feet.
14. Always see a podiatrist, a foot specialist, to take care of your feet, and notify them if you see that a problem area is not healing well.
I ( Dr. Burton S. Schuler) have been a professional member of the American Diabetes Association for about 35 years. And I have treated thousands of diabetics as a podiatrist, foot specialist in Panama City Fl. The one thing I know for sure is that there are three major problems, which all must come together at the same time, for the development of foot complications in the diabetic. They are
These three are known as the DIABETIC FOOT TRIAD. 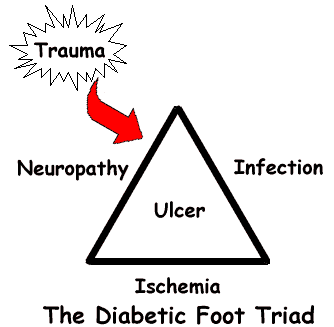 All three normally must be present in order for the possibility of an ulcer to occur (skin break down) which then can lead, to an infection (gangrene) which then can lead to an amputation. I say possible, because beside the TRIAD having to be present, the patient must also sustain some type of ongoing trauma or insult (precipitation factor) to their feet, to help trigger the infection phase. Because a person is a diabetic they are more prone to get the TRIAD, and then develop foot complications.
All three normally must be present in order for the possibility of an ulcer to occur (skin break down) which then can lead, to an infection (gangrene) which then can lead to an amputation. I say possible, because beside the TRIAD having to be present, the patient must also sustain some type of ongoing trauma or insult (precipitation factor) to their feet, to help trigger the infection phase. Because a person is a diabetic they are more prone to get the TRIAD, and then develop foot complications.
Ischaemia, which is a lack of blood, is a symptom of Peripheral Vascular Disease, in the foot, caused by an abnormally high Glucose level; which can then lead to skin break downs (ULCERS). If the blood supply to the foot is reduced sufficiently, minor wounds may not heal and the patient may have pain at rest due to the lack of oxygen to the foot. Ischemia can also be caused by CALCIFICATION of THE ARTERIES, which can be due to long term non-controlled diabetes, where the large blood vessels have an abnormal buildup of materials that blocks the flow of blood to the foot. Microangiopathies, which occur in the smaller blood vessels, known as the arterioles and capillaries is another cause of ischemia, and is prone to any blockage caused by diabetes. Because of these blockages the blood vessels can not transport enough blood to respond to any injury of the foot and or toes. Hence causing the start of various complications.
In the normal foot that has a normal glucose level and has normal feeling, small wounds or infections are distinguish by the amount of discomfort they present and are treated according. They almost always heal quickly without complications. In the long standing diabetic foot that has lost its feeling, a tiny cut may turn into a major problem because the patient can’t feel the problem. Nerve paralysis of the tiniest of the muscles (intrinsic) of the feet causes a muscle imbalance which results in the metatarsal heads of the foot being pushed down abnormally, and with a Hammering of the Toes taking place. These imbalances can become one of the precipitation factors that can start the break down of the skin.
If the precipitating factors are not controlled, infection can occur. In diabetic patients who have Circulation Disease and/or Nerve Damage, the presence of these precipitating factors can be the “smoking gun” that leads to infection, gangrene, amputation, or worst. The good news is that if you do get control of the precipitating/aggravating factor, this nightmare can be avoided. By determined treatment of any sign of any infection and by getting rid of the basis of any type of trauma to the foot, you have a much better chance of avoiding a foot infection.
To have a full blown infection which can lead to amputation you must have an on going insult to the foot. Some of them are repeated trauma caused by abnormal pressure in the foot, like from the metatarsal heads constantly pushing down or Ingrown Toenails constantly digging into the flesh; abnormal shoe pressure irritating, or burns caused by over-the-counter corn medication, or heating pads.
Panama City Fl podiatrist , foot doctor Dr. Burton S. Schuler, explains what a paper clip, a safety pin, a Lego block, a key, a hair pin, a rock, and a dime all have in common? They were all undetected foreign objects found in the shoes of people with diabetic neuropathy.
What Is Diabetic Neuropathy?
Diabetic neuropathy is a nerve disorder most commonly caused by the high levels of sugar in the blood. It represents the most common complication of diabetes. It is also the major contributor of the triad of diabetic neuropathy, Peripheral Vascular Disease and infection, which are the primary causes of all chronic foot diabetic ulceration that can lead to amputation. In fact in over 20 years in private practice I can not ever recall seeing a severe diabetic foot ulcer without diabetic neuropathy being present. As such they represent an ongoing health problem to the public of major importance. The most common form of diabetic neuropathy seen is known as “distal symmetrical polyneuropathy.” In layman’s terms this means the nerves affected are the far reaching nerves seen in the hands and feet, normally on both right and left sides, involving more than one nerve. People with diabetes can develop nerve problems at any time. Significant clinical neuropathy can develop within the first 10 years after diagnosis of diabetes and the risk of nerve damage increases the longer the patient is a diabetic. It has been published that as high of 60% of diabetics have nerve damage. Diabetic neuropathy emerges more commonly in patients over 40 who are smokers and who don’t keep their blood sugar under control.
What Causes Diabetic Neuropathy?
Many factors have been mentioned in medical literature as possible causes of diabetic neuropathies, but scientists do not know exactly what causes the condition. However, several factors are likely to contribute to the disorder. They are high blood sugar levels, disease of the blood vessels, high lipid levels (cholesterol and triglycerides), environment and genetic consideration. Far and away the common cause is high blood glucose, a condition that causes chemical changes in nerves. Again, we don’t know why high glucose affects the nerves, but we do know that it does. Studies have shown that high glucose levels affect many chemical pathways to the nerves, causing a build up in the nerve of a chemical known as sorbitol while decreasing the chemical called myoinositol. Several scientists feel this may be the “missing link” in the ultimate treatment of diabetic neuropathies, but as of now no one is sure.
High blood glucose also damages large and small blood vessels that carry oxygen and nutrients to the nerves. If there is not enough blood being sent to the nerve, the nerves ability to work will be effected. That is why it is so important that the blood supply to the feet and legs in a diabetic not be hampered.
Inherited factors also come in to play, but at the present time no one knows exactly why.
About the Author: Dr. Burton S. Schuler foot doctor, foot specialist, podiatrist of Panama City, Fl and the director of the Ambulatory Foot Clinics Podiatric Pain Management Center and is a leading authority on the Morton’s Toe, Long Second Toe and it associated problems. He is the author of the newly published book about The Morton’s Toe, Why You Really Hurt: It All Starts In the Foot. The book is published by the La Luz Press, Inc and is disturbed national by the Cardinal Publishing Group. Why You Really Hurt: It All Starts In The Foot, is the story of how one bone in your foot could be the real reason for pains thru out your whole body. It is important because it offer the public new information about why millions of people suffer everyday with aches and pains, and offers new hope to get rid of problems they believed they would have to live with forever. It literally can be the “medical missing link”
Dr. Schuler, graduated from the N. Y. College of Podiatric Medicine in 1975 at the age of twenty-four, and has been in private practice ever since. In 1982, he published his first book, The Agony of De-Feet: A Podiatrist Guide to Foot Care. During his thirty-five year professional career, he has written for Collier’s Encyclopedia and various podiatric journals and publications. He has been interviewed by The New York Times, First in Women, and other publications. Dr. Schuler has appeared on hundreds of radio and television programs both here and aboard. He is a Diplomate of the American Academy of Pain Management, and the National Board of Podiatric Examiners. Dr. Schuler is certified as a wound specialist from the American Academy of Wound Management. His professional and civic accomplishments have earned his inclusion in the 1999-2002 Who’s Who in America (Marquis).
Type I
By definition the only treatment for Type I diabetes, is the on going injection(s) of insulin. Before Insulin was discovered in the early 1920’s by two Canadians, Frederick Grant Banting and Charles H.Best, most people with IDDM died within a short time of getting Diabetes because the “beta cells” of their pancreas were destroyed. Please remember insulin is not a cure for diabetes. Beside the insulin, patients with Type I diabetes must also follow a specific personalized diet, with daily checking of blood sugar, and of course exercise.
Type II
In NIDD you have less insulin than the normal person, because even though the pancreas is producing some insulin, via its working “beta cells” there is too little of it (insulin) for your body to work properly.
The aim of the treatment for those with Type II is to supplement the amount of insulin that is already in your body in order to prevent a full blown case of diabetes from occurring. The basic preventive technique like Type I, is to diet, exercise, and check your glucose level. Many Type II patient’s also have to take pills called “oral hypoglycemic agents” to lower their sugar level, by exciting the beta cells in the panaceas to make more insulin.
If is vital to keep control of your NIDDM/Type II diabetes. If not, over a period of time you will be prone to having any and or all of the following symptoms; cold hands and feet, burning and/or numbness of the feet or hands, poor vision, increased thirst, increased urination, and sores that are slow healing or won’t heal.
THE TEAM APPROACH
Diabetes is a multiple system disease. This means it is affecting many parts of your body at the same time. You must get the right person to handle the specific part of your body. Besides your family doctor you may want to be under the care of a diabetic specialist called an endocrinologist. He is a doctor who spends most of his day dealing with diabetics. I would encourage all patients especially Type I, to see an endocrinologist at least once to evaluate your condition, unless you are already under the care of an internist, and there appears to be no problems in your treatment. Other members of this team would be a kidney specialist, and eye specialist, and a foot specialist. Also if you are having an on going problem with your diet, an dietitian would be of great use.
Thousands of people live long, totally normal lives with Diabetes, but it does depend on how well they take care of themselves.
The glycated hemoglobin test is by far the most important test for controlling your sugar. It is often called the glycosylated hemoglobin test or hemoglobin (A1C) and is a measurement of the overall control of the diabetic for the previous two to three months. Most diabetic specialists feel it is now the single most important blood test for known diabetics. The American Diabetes Association recommends that if you are a diabetic, this test be taken every 3 months. For patients who are not yet diagnosed with diabetes, it is becoming more popular for making the initial diagnosis of Diabetes.
The fasting blood sugar (FBS) test, which is still the mostly commonly performed test for Diabetes, does not reflect the true picture of diabetic control over a long period of time. The FBS only measures the level of sugar in the blood at the moment it is taken from your finger or arm. Patients have been known to “fake” the results of their FBS by staying on their diet and medication (when they normally won”t) for several days leading up to the FBS, in order to have a more normal result, when in fact their glucose (sugar) levels were out of control. You can not fake the results with a glycated hemoglobin test because it is based on 90 days, not an instant like the FBS.
HOW IT WORKS
The glycated hemoglobin test measures how much glucose is attached to hemoglobin cells, the part of the blood that carries oxygen. As the hemoglobin floats around in the blood, it picks up glucose in about the same proportion as the glucose that exists in the bloodstream. If your blood glucose is generally running high, the hemoglobin will have more “glucose coating” (glycosylization). If your glucose generally runs low, it will have less. Since the red blood cells have about a two to three month life span in the body before they are recycled, we can measure the “glucose coating” of a sample of hemoglobin. This gives you an approximate average of glucose control over the last two to three month period.
What is the goal of the glycated hemoglobin test?
Every person, whether or not he or she has diabetes, has a certain amount of glycosylization present. Because of more sugar in their blood, people with diabetes have a greater amount of glycosylization present. A low result on the glycated hemoglobin test is a good result. If your test is in the good control category, slot machines online for real money you can be satisfied that your diabetes management plan is working well. If results are in the marginal category, some fine tuning of your treatment plan may be needed. A poor result can be improved. This test gives you valuable feedback on how well you are controlling your diabetes. It can also let you know when to work on improving your diabetes management.
It”s important for you to remember that normal values for the glycated hemoglobin test may vary from laboratory to laboratory, because different laboratories use different procedures to perform the measurement. Be sure to ask for the “normal” range for that particular lab. But a goal of 7 or less is what you want. It”s best to have the tests done by the same laboratory so you can compare the results from one test to the next to note the progress you are making. Your physician will help you determine your goal range for glycated hemoglobin. If you are Type I or Type II diabetic, you should be having this test every 90 days; there is no reason that you should not. If your physician is not running the glycated hemoglobin test on you every 90 days ask him why.
Dr. Burton S. Schuler is a foot doctor, foot specialist (Podiatrist), of Panama City, Fl and the director of the Ambulatory Foot Clinics Podiatric Pain Management Center. He is also the author of the new book Why You Really Hurt: It All Starts In The Foot he has been a member of the American Diabetes Association for over 25 years.
There are two major types of diabetes. Type I, or insulin-dependent diabetes (IDDM), is when the cells that make insulin in the pancreas (beta cells) are totally destroyed. It is generally felt that this destruction of the beta cells is probably an autoimmune reaction; which means that the body’s own immune system turns against the body and kills these pancreatic cells that produce insulin. Because the beta cells are killed off, the pancreas then produces little or no insulin, with an end result of an unhealthy buildup of glucose in the blood. The person with Type I Diabetes must have daily injections of insulin to live. As of now, science is not sure why the body turns on itself to attack the insulin producing beta cells, but they think that both inheritance and viruses may be the causes. According to the American Diabetes Association, Type I (IDDM) accounts for 5 to 10 percent of diagnosed diabetes in the United States. It is most commonly seen in childhood, thus the term “juvenile-onset”, but it also can occur to age 40 and above. The typical patient with Type I is lean as compared with the more obese patient in Type II. Symptoms of Type I usually develops very quickly, although destruction of the beta cells may have started months, or years, before. Symptoms of Type I includes increased thirst, urination, hunger, and weight loss. Increased tiredness and blurred vision, are also symptoms. If the patient is not diagnosed properly and treated properly with insulin, then the patient is exposed to having all of the complications of diabetes and being prone to premature death.
Type II, or non-insulin-dependent diabetes (NIDDM) is by far the most common type of diabetes. Ninety to 95 percent of people with diabetes have NIDDM. Type II diabetes usually appears in adults who are 40 and above and is most common in adults over 55, that is why it is also referred to as “adult-onset diabetes” or “maturity-onset diabetes”. It affects more women than men. The vast majority of Type II patients, about 80%, are overweight.
In Type II diabetes, one of two things normally happens: 1. the pancreas usually produces insulin, but for some unknown reason the body cannot use this insulin becoming “resistant” to it, or 2. not enough insulin is produced by the pancreas. Regardless, in either case, the end result is the same: an abnormal buildup of glucose in the blood with a resulting inability of the body to properly use its main source of fuel.
The symptoms of Type II Diabetes tend to develop more slowly and are more vague and not as clear-cut as the symptoms in Type I. The most common symptoms of Type II include increased tiredness and or illness, increased urination at night, unusual thirst, unusual weight loss, blurred vision, increased infections, and abnormal healing time of sores. Treatment can vary from diet, exercise, weight loss, to oral drugs that increase the release of insulin. In some cases Type II diabetes can even be treated with insulin.
A third type of diabetes, called gestational diabetes, can appear in 3% of women during pregnancy. Gestational diabetes usually disappears once the pregnancy is over. Those women who do get gestational diabetes have a higher than normal risk of having Type II diabetes later in life.
Dr. Burton S. Schuler is a foot doctor, foot specialist (Podiatrist), of Panama City, Fl and the director of the Ambulatory Foot Clinics Podiatric Pain Management Center. He is also the author of the new book Why You Really Hurt: It All Starts In The Foot
| What is Diabetes? | Circulation Problems |
| Types of Diabetes. | Complications |
| Important Blood Test | Self Care |
| Treatments | Important Press Release |
| Nerve Damage | Advances in Treatment |